Managing Rosacea
- Greta Ryan

- Aug 30, 2021
- 6 min read
Updated: Oct 1, 2023
Rosacea is complex, commonly misunderstood, and under-diagnosed - but it's not an uncommon skin condition. Having rosacea is usually a lifelong thing, and good management is important. Without proper understanding and guidance though, it's easy to get it wrong - so let's talk about it!
What is Rosacea?
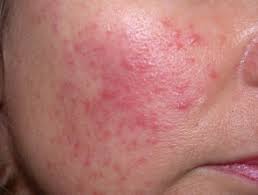
Rosacea is a chronic skin condition that results in persistent redness/flushing, visible blood vessels, sensitivity and often small, red, pus-filled bumps on the face (this feature can sometimes result in a misdiagnosis of acne). Some forms of rosacea can also result in swelling and thickening of the skin. Occular (eye) symptoms can also occur, and can be serious - if the eye area starts to become affected, it's important to seek medical intervention as soon as possible.
Rosacea usually starts to appear between the ages of 30-50.
Symptoms usually appear in the cheeks, nose, forehead and chin. In women, it's more common in the cheeks and chin. In men, more often symptoms are focused around the nose.
Rosacea is more common in women, but tends to be more severe in men - this is now thought to be because men usually seek treatment far later than women, and therefore allow their symptoms to worsen considerably more before treating the rosacea.
Historically, it was believed that rosacea affected lighter skin more often than darker skins - but in recent times, it's been understood that rosacea is under-diagnosed and often missed in darker skins. This is possibly because the higher melanin content of darker skin can hide some of the vascular components of rosacea (eg. redness, visible blood vessels) - and possibly it's also a result of poor education for skincare providers around recognising rosacea in darker skins.
Rosacea is usually a lifelong skin condition, so it's important to understand that it cannot be "cured". The goal with rosacea is management - and as much reduction of symptoms as possible.
The Subtypes
There are several different ways that rosacea can present, and these have been broken down into subtypes:
Erythematotelangiectatic Rosacea (facial redness, flushing, and visible blood vessels)
Papulopustular Rosacea (small, red/inflamed bumps that can be pus-filled or not)
Rhinophyma (thickening of the skin on the nose)
Occular Rosacea (affecting the eye area, can result in: dry eyes, itchy/sensitive eyes, bloodshot eyes, gritty sensation, corneal damage and diminished vision in serious cases)
These subtypes often occur in conjunction with eachother, so you can have more than one subtype - for example, one might have papulopustular rosacea alongside occular rosacea. Or Erythematotelangiectatic rosacea alongside rhinophyma.
The subtypes are just one classification system for rosacea - there is also the "phenotype" classification system, but for the purposes of this article I decided to stick with the subtypes.
How does it happen?
Short answer: we're not sure.
The exact cause (or pathophysiology) of rosacea is still not entirely known - but we are building a clearer picture of the different factors that contribute to it.
The best answer to this question is that rosacea is multifactorial, meaning there are many factors that contribute to both its development and severity. A few of these factors are believed to be:
Genetics
Because there are multiple factors implicated in rosacea, it doesn't have a clear pattern of inheritance. That said, some studies suggest that people with rosacea are more likely (one study quoted this to be four times more likely) to have a family history of rosacea. This could be in part due to genetic factors, but it may also be related to environmental factors that are shared by families.
Environment + Lifestyle
A clearer picture is emerging of exactly which environmental and lifestyle factors can worsen rosacea and trigger flare ups. These things are not believed to be the cause of rosacea, but they certainly have been shown to worsen rosacea symptoms. You'll find the most common environmental/lifestyle triggers listed further down in this article, when we talk about "trigger avoidance".
UV Exposure
Again, this factor is not thought to cause rosacea, but it has been shown to significantly worsen symptoms of rosacea and contribute to its severity. This is partly due to the damage that UV exposure causes to the skin, increasing inflammation and sensitivity - but also due to the ability of UV to upregulate (or stimulate) VEG-F: Vascular Endothelial Growth Factor. VEG-F promotes formation of blood vessels in the skin, and therefore can increase redness, flushing, and visible blood vessels in rosacea.
Abnormal innate immune responses
In recent times, the immune system has been looked at as a possible piece of the rosacea puzzle. Rosacea affected skins have been found to have abnormal innate immune responses, suggesting that this may be a factor in the disease process of rosacea. This theory is however, yet to be conclusively confirmed.
Dysbiosis of the skin microbiome and gut microbiome
Several microbiome related factors have been suggested to be associated with rosacea, including SIBO (small intestinal bacterial overgrowth), and IBS (Inflammatory Bowel Disease). Dysbiosis of the skin microbiome has also been looked at, however studies linking these factors to rosacea are not yet conclusive, so again - this is just another theory for now.
Demodex Mites
Last, but not least - demodex mites. These tiny mites live on our skin - we all have them, but in rosacea-affected skin, they tend to be found in significantly greater numbers. Demodex mites were suggested as a possible cause for rosacea about a decade ago, then dismissed - but in the last few years the theory has been revisited. When demodex mites die, they release bacteria onto the skin - this process can trigger immune responses that cause redness and inflammation.
One aspect of the Demodex theory, is that because demodex mites thrive by feeding on oils in the skin, they could be a possible explanation as to why rosacea usually flares up in response to oily/occlusive skincare products.
All in all, there are many factors that are thought to play a role - reinforcing the conclusion that rosacea is multifactorial and there are many pieces to the puzzle.
So, how do I know if I have rosacea?
It's really important to get a proper diagnosis from your GP or dermatologist - many other skin conditions can look like rosacea, but behave quite differently (and require different care), so don't try to self-diagnose.
If you have confirmed that you do in fact have rosacea, it's time to learn how to manage it.
Medical Intervention
In moderate-severe cases of rosacea, medical intervention is often required. It's important to see your doctor if your rosacea is becoming severe, and especially if you develop any occular (eye) symptoms.
However in ALL cases of rosacea, severe or not - trigger-avoidance and a good skincare routine at home, can be incredibly helpful in managing symptoms.
1. Identify your triggers, and avoid them
Common "triggers" that cause rosacea to flare up, include:
- UV exposure from the sun
- Stress
- Heat (hot weather, but also - spas, saunas, heavy exercise)
- Alcohol
- Spicy foods
- Certain skincare products (we'll go through what to avoid, further down)
Being mindful of avoiding your triggers, will help to reduce rosacea flare-ups, making it easier to manage.
2. Your skincare at home is a powerful tool for managing your Rosacea
Topical skincare can make an enormous difference to rosacea. It can reduce inflammation, manage flare-ups, improve hydration, and strengthen delicate skin. The key of course, is getting it right.
Below, is a typical skincare routine we give to our clients who are dealing with rosacea. Every skin will be slightly different, but this is a tried and tested routine that we have found to be successful in managing rosacea:
AM (in order of use)
- Gentle cleanser. Avoid cream or oil cleansers, and go for a gentle gel/foam. Mild Clean by Aspect Dr (gel) or Calmwise by Medik8 (foam) are perfect options.
- Hydrating serum. I tend to recommend Optiboost by Aspect Dr, or Hydr8 B5 by Medik8.
- Vitamin B serum. Multi B Plus by Aspect Dr is the ideal vitamin B serum for rosacea - it's lightweight, and contains every form of vitamin B.
- Lightweight moisturiser. Heavy, occlusive moisturisers will also often worsen rosacea, so it's important to avoid these. Go for something lightweight, like ReBalance by PCA Skin.
- Physical/"mineral" sunscreen. This means a sunscreen that uses zinc oxide and titanium dioxide as its active UV blockers. We recommend physical sunscreen for rosacea because it has anti-inflammatory properties, and has a lowered chance of irritation vs some non-mineral UV filters. Sheer Zinc by Dermaquest is a fantastic mineral sunscreen, and is lightweight/non-greasy.
PM (in order of use)
- Gentle cleanser. (same as AM)
- Vitamin B serum. (same as AM)
- Vitamin A serum. I tend to recommend Calm by Osmosis to begin with, and then to move up to the PCA Skin Retinol For Sensitive Skin which is also fantastic.
- Lightweight moisturiser. (same as AM)
Avoid Oils In Your Rosacea Skincare
Rosacea does NOT respond well to topical oils. Often, rosacea causes chronic dehydration & dryness, so many people turn to oils to remedy this - but in reality, oils usually only worsen the rosacea symptoms. Heavy, occlusive products will also often worsen rosacea, so it's important to avoid these too.
Avoid AHA/BHAs
A common feature of rosacea is sensitivity, and a tendency toward barrier impairment. For this reason, we tend not to recommend AHAs (like glycolic acid) and BHAs (like salicylic acids), with very few exceptions.
In terms of skin treatments, vitamin A infusion peels can be very beneficial in strengthening the skin and managing inflammation - once you are on a good skincare routine at home.
If you're struggling with your rosacea, don't go it alone - book a free skin consultation with us for some honest guidance and support.
If you're unsure if you have rosacea or not - go see your GP or dermatologist first, for a proper diagnosis.









Comments